Mississippi hospitals preparing for ‘tidal wave’ of new Coronavirus cases
Amid first reported death, Mississippi hospitals brace for COVID-19 ‘tidal wave’
by Erica Hensley, Mississippi Today
March 19, 2020
A day before Mississippi reported its first death due to coronavirus — a Hancock County resident who died at a Louisiana hospital — the head of the state’s busiest emergency department sent a message: We’re preparing as best we can, but it won’t be enough.
Public health experts are frantically monitoring COVID-19’s path and estimating how many Americans the new respiratory virus might infect, and of those, how many will become severely ill. The answers to these questions relies on how effectively the country “flattens the curve” in the coming weeks to prevent a quick spread that could overburden the nation’s health care system.
Dr. Thomas Dobbs, the state’s top health official, said this week that Mississippi is currently seeing “low-level community spread,” meaning the virus is moving through communities, no longer directly tethered to travel.
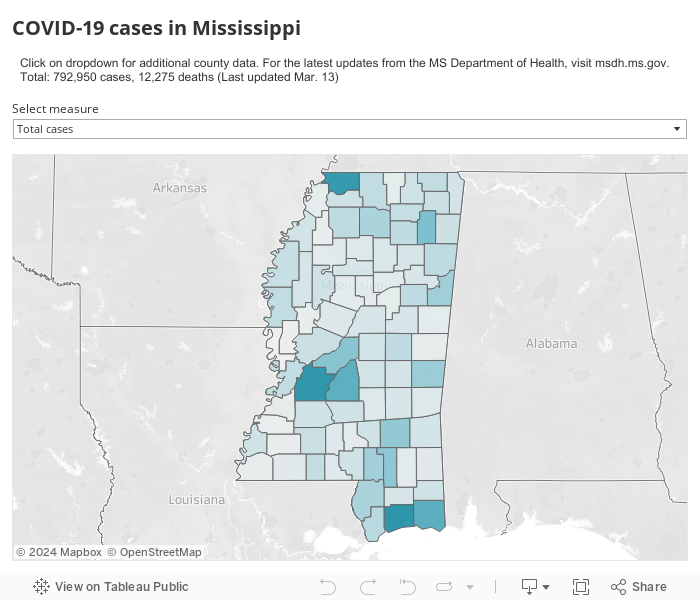
Since the first case was diagnosed last week, Dobbs has repeatedly urged Mississippians to help prevent spread now so as to not overwhelm our health care system later. As of March 19, one death and 50 cases out of 602 tests have been reported by the state health department, peppering the whole state with infections. Nationally, the country surpassed 10,000 cases this week and 172 deaths.
var divElement = document.getElementById(‘viz1584637200214’); var vizElement = divElement.getElementsByTagName(‘object’)[0]; if ( divElement.offsetWidth > 800 ) { vizElement.style.width=’700px’;vizElement.style.height=’627px’;} else if ( divElement.offsetWidth > 500 ) { vizElement.style.width=’700px’;vizElement.style.height=’627px’;} else { vizElement.style.width=’100%’;vizElement.style.height=’727px’;} var scriptElement = document.createElement(‘script’); scriptElement.src = ‘https://public.tableau.com/javascripts/api/viz_v1.js’; vizElement.parentNode.insertBefore(scriptElement, vizElement);
This week, leaders of the state’s largest and only academic hospital warned of widespread coronavirus cases. Because there is no vaccine or drug treatment for the virus, the burden of mitigating the pandemic will largely fall on communities and hospitals.
University of Mississippi Medical Center officials said they’re using the full force of the academic center’s resources to prepare for the unprecedented coming wave of patients by preserving protective medical equipment for health care providers and keeping people who don’t need high-level care out of the hospital. For the latter, UMMC officials said they’re developing an in-house test to increase diagnostics across the state, expected in the coming weeks. Meanwhile, the hospital is launching a telehealth smartphone app and live telephone line that can treat non-emergency COVID-19 patients remotely. Those services are expected in the coming days, officials said Wednesday.
Dr. Alan Jones, chair of UMMC’s Department of Emergency Medicine, urged Mississippians to heed calls to stay at home and help prevent the virus spread, echoing both Dobbs and Gov. Tate Reeves alike, both whom have warned that Mississippi’s health care system risks being overrun if the state doesn’t temper the viral spread.
“We are ramping up all of our contingency plan to be prepared for a tidal wave of patients that we know is about to hit us,” said Jones, who leads the hospital’s new coronavirus clinical response team.
“Some of the reason that you’re being asked to alter your lifestyle – to stay at home, to social distance, to not go to restaurants, keeping kids out of school – all these things that disrupt our life, really are not aimed at preventing, per se, people from getting the virus,” he said.
“Because we know people are going to get the virus, it’s a very effective virus. It’s really to give health care a fighting chance.” He added most people will recover and won’t need hospital care. “We can’t stress enough that we need people to allow us to do our job and take care of the sick, sick patients, and not everyone.”
Health care groups are starting to sound the alarm for overcrowding risks, as well as medical staff and space shortages. Last month, the American Hospital Association wrote to Congress that the U.S. health care system was unprepared to handle coronavirus and needed financial help, specifically noting scarce protective equipment, isolation space and treatment rooms.
Health policy think tank Kaiser Family Foundation used national data to estimate how many Americans risk getting severely ill if they contract coronavirus, finding about 4 in 10 adults are at higher risk – 41 percent – due to age and chronic illness. Though most people who contract the disease will not become seriously ill, in Mississippi that percent is slightly higher at 44 percent, or 993,440 adults across the state.
Using the Kaiser Family Foundation estimate of 993,440 Mississippians at-risk of severe illness if they contract coronavirus and the most recent hospital bed counts available, Mississippi Today’s capacity analysis estimate the state has one hospital bed for every 83 at-risk person, and one intensive care unit bed for every 1,182 at-risk person.
A Harvard study released this week modeled on-the-ground risk at different points of virus control, depending how effectively the country controls spread in the coming weeks. The model breaks down the U.S. into hospital areas, with Jackson and Memphis regions covering most of Mississippi.
According to Harvard’s research, if 40 percent of adults are infected with coronavirus over 12 months, the model’s “moderate scenario,” Jackson hospitals would need to more than double its capacity, by 324 ICU beds based on average use. Assuming every ICU bed is free, Jackson would still need 67 more. In the same scenario, Memphis would be hit much harder needing to scale up by six times its current available ICU capacity, over 650 beds. Assuming all ICU beds are free, Memphis would still need 263 more beds to handle COVID patients that need hospital care.
The models show Meridian and Oxford as the only hospital regions in the state that would not need to expand current capacity for COVID-19 patients. These estimates are based on number of available beds at any given time, potential surge of patients, and number of people who might need hospitalization, which are based on estimates similar to the Kaiser (map above) predictions.
While Mississippi has fewer people and less crowding than other parts of the country, the state also has far fewer medical epicenters and hospital beds, and on any given day, a higher rate of sick people who are using those beds and higher proportion of people without insurance coverage who lack access to care altogether.
Already, Mississippi sees the highest death rate for flu across the country. As a preventable illness, it can be seen as a metric for a region and its hospitals’ capacity to handle flu-like disease spread. Mississippi sees 26 deaths to flu per 100,000 people, compared to the nation’s rate of 15 per capita.
The state’s actual level of preparedness is hard to measure, though officials have assured citizens they have enough tests. After activating a state of emergency and calling up the National Guard, Reeves has said that coronavirus tests need to be rationed for “hospitalized patients, health care workers with symptoms and vulnerable citizens with fevers.”
Reeves added: “Our top risk is that the U.S. health care system would be overwhelmed. Please help us keep it secure.”
Scanning the larger hospital websites, almost every one shows a red banner stretching across its homepage assuring the public of the hospital’s preparedness. But a closer look at the numbers paints another picture more in-tune with Jones’, emergency medicine director at UMMC, and national warnings that supplies will run out, and are already in short supply in parts of the country.
Many hospitals, including half in Jackson, wouldn’t provide exact counts when Mississippi Today asked this week about capacity, and the Mississippi State Department of Health officials did not provide specific numbers, though they track bed availability. MSDH hasn’t released an updated full hospital capacity accounting since 2015 when the state had 10,592 total hospital beds, not including those dedicated to psychiatric care.
In 2015, 1,223 of those were intensive care unit beds, devoted to high-level care like the kind needed for hospital-based COVID-19 treatment – 766 of which were for general use, called “medical-surgical,” not devoted to pediatrics, neonatal, cardiac or burn specialties. Those numbers indicate in 2015, 12 percent of that state’s overall beds were devoted to ICU care, with 7 percent open for general ICU medical-surgical use. Since those numbers were released in 2015, four hospitals have closed in the state.
The health department’s 2019 hospital directory, which represents the best count for current beds short of an updated hospital report, shows the state had 12,014 non-psychiatric hospital beds, mostly devoted to acute inpatient care. If the proportion of ICU beds across the state remained stable since 2015, there are about about 840 general-use ICU beds across the state currently.
For those that did respond, most of those above a 100 bed count, averaged between 5 and 14 percent ICU capacity, out of total beds. One 200-bed hospital has 24 ICU beds and a 268-bed hospital has 13. For those that responded, the average percent of ICU beds out of total beds was 10, which tracks with national rates.
Any given time, about two-thirds are in-use in the state’s busiest hospital region in Jackson, according to 2018 data used in the Harvard model. The state’s largest hospital and the only offering Level 1 trauma care, UMMC, has 93 ICU beds that are usually at-capacity.
“We run full everyday, that’s the nature of who we are in the state of Mississippi,” Kevin Cook, CEO of UMMC’s health system, told reporters Wednesday.
Using current ICU capacity broken into regions, based on data from the Harvard study, Mississippians could have access to around 1,500 beds across the state and in neighboring areas (not accounting for use at any given moment).
- Jackson and surrounding areas: 410 ICU beds total
- Memphis metro: 540 ICU beds
- Mobile metro: 280
- Tupelo: 100
- Hattiesburg: 85
- Gulfport: 80
- Meridian: 57
- Oxford: 29
For a moderate outbreak nationwide, 1 million people would need hospital care – 200,000 needing ICU care, according to Johns Hopkins University researchers. That’s more than four times the number of total ICU beds currently in the U.S., which the national hospital association puts at around 48,000.
In Mississippi, where the number of confirmed cases went from zero to 50 in one week, statistical models show we need to increase our capacity to handle potential patient surge. Regionally, Georgia has struggled with sudden waves of patients in its regional hospitals, as well as staff shortages while doctors, nurses and staff were quarantining at home after potential exposure. As of Wednesday, Georgia’s confirmed cases stood at 197, one of the hardest hit states regionally, along with Louisiana, which has seen stark case growth over the last week.
The state’s medical association and health department Thursday urged all physicians across the state to cancel all elective care during the pandemic, to prevent the disease spread and preserve health care resources, according to a letter obtained by Mississippi Today. Shortly after the letter went out on Thursday, the state health department released a statement telling physicians they “must” delay non-essential and non-urgent medical care.
MSMA Recommendation on Elective Surgery 031820 (PDF)
MSMA Recommendation on Elective Surgery 031820 (Text)
DV.load(“https://www.documentcloud.org/documents/6813520-MSMA-Recommendation-on-Elective-Surgery-031820.js”, {
responsive: true,
container: “#DV-viewer-6813520-MSMA-Recommendation-on-Elective-Surgery-031820”
});
MSMA Recommendation on Elective Surgery 031820 (PDF)
MSMA Recommendation on Elective Surgery 031820 (Text)
UMMC officials Wednesday confirmed that two of Hinds county’s six confirmed cases were a UMMC student and a nurse, which caused other staff to be quarantined as well. Medical students’ clinical rotations have been cancelled, officials said. “We have precious few health care providers, we have precious few (personal protective equipment) that we can use,” added Jones, head of emergency department. “And we need to conserve those resources the best we can.”
He added that UMMC is trying to provide advice to clinics across the state about how to prepare patient flow and protections, adding no health care system is prepared to deal with a pandemic.
“We are working with clinicians as closely as we can, communicating as rapidly as we can, and getting as prepared as we can. We know it won’t be enough,” he said. “That’s just what we’re facing. But we will be as prepared as we can be.”
For COVID-19 preparation, other factors inform hospitals’ readiness, such as the protective equipment like masks, gloves and gowns mentioned by UMMC officials; number of ventilators and heart-lung machines that can help people breathe when they can’t on their own; and in worse-case scenarios, negative-pressure rooms that help reduce spread of contagious disease by keeping the air in the room, rather than circulating to the rest of the hospital.
The state’s hospital association is working to help the state’s health care system bulk up their emergency plans, including increasing bed capacity and ventilators where possible, says Joyce Pearson, director of emergency preparedness for the Mississippi Hospital Association.
“Hospitals are always working on their emergency preparedness plans, including surge capacity for beds as well as ventilators. Mississippi could possibly need more hospital beds, and our current crisis does make it critically important that Mississippians use the health care system appropriately, take precautions to keep themselves well, and follow social distancing guidelines to stop the spread of the disease. The social distancing guidelines are being put in place to help prevent that need,” she said in an email.
There are currently 160,000 ventilators in the U.S., with 8,900 on reserve. In moderate outbreak scenarios, at least 200,000 Americans would need ventilator care.
Only UMMC and 14 smaller regional hospitals responded to questions about negative pressure rooms and ventilators on-hand. UMMC currently has 40 negative pressure rooms, and can scale up to about 100 if needed, according to officials. The hospital is planning to move all COVID-19 patients to one unit to prevent spread and keep ICU beds available for other critically ill or injured patients, and said they could have several hundred ventilators in the near-future, pulling from all hospital sources and adapting equipment.
The regional hospitals across the state that responded have an average of 10 negative pressure rooms per hospital. On average, hospitals larger than 100 beds tend to dedicate 10 percent to ICU. Hospitals that responded to on-hand ventilator count had anywhere between 1 and 86, averaging 17 each.
Click here to enter Mississippi Today’s COVID-19 Resource Portal.
This article first appeared on Mississippi Today and is republished here under a Creative Commons license.